Tooth wear rarely starts as a “crown everything” problem. It starts as a biology, biomechanics, and timing problem. Patients may present with flattened cusps, cupped posterior teeth, shortened anterior edges, loss of vertical dimension, sensitivity, or esthetic concerns. The old reflex was often full coverage. The newer question is better: how much healthy tooth can still be preserved while rebuilding function? That is why occlusal veneers have become such an important part of modern worn dentition treatment.
In plain terms, occlusal veneers are thin bonded restorations that rebuild the chewing surface of worn posterior teeth without covering the entire tooth the way a full crown does. A recent scoping review describes an occlusal veneer as a type of partial coverage restoration with a non-retentive preparation design and reduced ceramic thickness. That definition matters because it captures the real advantage: occlusal veneers are meant to be adhesive, conservative, and tissue-preserving by design.
That conservative mindset is not just academic. A systematic review on tooth wear concluded that worn dentition treatment should be reversible, adhesive, and additive whenever achievable. Another foundational review on biologically based tooth wear management argued that the focus should stay on long-term tooth survival, not just restoration survival, and specifically urged clinicians toward additive rather than destructive full-mouth reconstruction whenever possible. That is the philosophical home of occlusal veneers.
Associated Dental Lab’s published guidance lines up with that same philosophy. ADL repeatedly frames restorative success around preserving enamel when possible, choosing an adhesive pathway for partial coverage cases, using deep margin elevation when margins are sulcular and isolation is realistic, and reserving full crowns for cases that truly need circumferential coverage and ferrule. In other words, the lab logic supports the clinical logic: occlusal veneers beat full crowns when a conservative bonded solution still has the biology, isolation, and material support to succeed.
What occlusal veneers actually are in worn dentition treatment
A simple definition
For a general audience, the easiest way to understand occlusal veneers is to compare them with full crowns. A full crown wraps around the whole tooth after substantial reduction. Occlusal veneers usually restore mainly the worn biting surface and selected cuspal areas, preserving far more of the remaining tooth. In wear cases, that difference is often the difference between additive dentistry and subtractive dentistry.
Why they fit wear cases so well
Wear cases often leave clinicians with a paradox: the tooth is damaged, but much of the remaining enamel and axial structure may still be worth preserving. A patient may have severe occlusal wear yet still have enough peripheral enamel and enough sound tooth to support a bonded posterior restoration. That is where occlusal veneers can shine as worn dentition treatment and as tooth wear restoration, especially when the goal is to rebuild lost volume rather than amputate the remaining tooth into a stump.
Why this is really about additive dentistry
Additive dentistry means restoring what was lost with as little additional removal as possible. That principle matters more in younger patients, erosive wear cases, bruxers with already-thinned teeth, and full-mouth rehabilitations where every millimeter of remaining enamel is precious. Occlusal veneers fit additive dentistry because they are designed to add back worn anatomy, not reflexively create a conventional crown prep just because the tooth is already compromised.
Why occlusal veneers can beat full crowns
They preserve dramatically more natural tooth structure
This is the biggest reason occlusal veneers can beat full crowns. A systematic review and meta-analysis comparing posterior onlays and partial crowns with full crowns reported no statistically significant difference in short-term survival or success at one and three years, while also noting that full crowns are the most invasive option. The same review cites classic data showing that full crown preparations remove about 67.5% to 75.6% of tooth structure, while onlays and partial crowns remove about 35.5% to 46.7%. That gap is enormous in lifelong restorative terms.
In practical terms, that means a clinician can often deliver a strong tooth wear restoration without spending the patient’s remaining tooth capital all at once. Full crowns still have an important place, but when occlusal veneers can deliver the needed strength and function, they often win simply because they cost the tooth less. That is a powerful advantage in worn dentition treatment, where many patients are already starting with a reduced structural reserve.
They fit the biology-first approach to wear
The biologically based literature on tooth wear management makes a simple point: the survival of the tooth matters more than the survival of any single restoration. That way of thinking favors reparability, maintenance, and staged care over aggressive full-coverage treatment whenever possible. Occlusal veneers align with that mindset because they preserve tooth structure and keep future options open. If a restoration needs repair or replacement later, the clinician is often still working with more remaining tooth than would be left after a full crown.
They are ideal for additive dentistry and vertical dimension rebuilding
Many wear cases are not just about one tooth. They are about re-establishing occlusal anatomy across multiple teeth, sometimes with a change in vertical dimension of occlusion. That is where occlusal veneers often outperform full crowns conceptually. Instead of cutting every tooth down to create uniform space, additive dentistry can create the needed restorative volume by building worn surfaces back up. Associated Dental Lab’s provisional guidance specifically identifies milled PMMA as a strong option for vertical dimension trials and longer-wear provisional phases, which makes it highly relevant to worn dentition treatment planning before definitive occlusal veneers are delivered.
They can keep margins more conservative
One of the hidden costs of full crowns in wear cases is margin placement. A full crown may force the clinician toward more circumferential reduction and sometimes deeper margins than the tooth or periodontium really wants. Associated Dental Lab’s margin elevation versus crown lengthening guidance repeatedly steers clinicians toward the least invasive design that meets strength goals, and specifically recommends adhesive posterior restorations when margins are sulcular, isolation is achievable, and ferrule is not mandatory. That logic often favors partial coverage over a full crown.
That does not mean every deep box becomes an occlusal veneer case. It means that when deep margin elevation can relocate a margin conservatively and a bonded restoration can still succeed, the clinician has a path that may preserve more enamel and avoid surgery. In the right wear case, that is one of the clearest ways occlusal veneers beat full crowns.
They are built for bonding, not just cementation
Associated Dental Lab’s resin cement guide makes an extremely useful distinction: first ask whether the case is mainly a retention case or a bonding case. ADL explicitly classifies veneers, inlays, onlays, partial coverage restorations, and short or tapered crowns as bonding cases. That is a perfect description of how occlusal veneers should be approached. Their success depends on adhesion, surface treatment, and isolation, not just on dropping a restoration onto a conventionally retentive prep.
When occlusal veneers are the better worn dentition treatment
Not every posterior wear case should receive occlusal veneers. But when several of the following features are present, they often become the more conservative and smarter option:
- The patient has moderate or severe occlusal wear but still retains useful peripheral enamel.
- The main problem is lost occlusal anatomy, not circumferential structural collapse.
- The case benefits from additive dentistry, especially when opening vertical dimension conservatively.
- Margins can remain supragingival, equigingival, or at least manageable with predictable isolation.
- The clinician can execute a true adhesive protocol for the chosen material.
- The tooth does not require full-crown ferrule for long-term survival.
- The occlusal scheme can be tested and adjusted thoughtfully before final delivery.
Those criteria are the practical overlap between the tooth-wear literature and ADL’s bonding, margin, and workflow guidance.
Cases that especially favor occlusal veneers
Occlusal veneers are often at their best in these scenarios:
- Posterior erosive wear with cupping and flattening, where axial walls remain largely intact.
- Generalized attrition where the restorative goal is to add back lost vertical anatomy across multiple posterior teeth.
- Full-mouth worn dentition treatment that uses PMMA prototypes first and definitive ceramics later.
- Cases where a minimal prep posterior restoration can stay largely in enamel and avoid a crown prep.
- Patients who are young enough that preserving future restorative options matters enormously.
That list reflects the broader trend toward reversible, adhesive, additive treatment in tooth wear management.
The biggest caveat: evidence is promising, but still not as deep as crown evidence
The enthusiasm around occlusal veneers should be balanced with honesty. A 2025 scoping review of posterior partial coverage restorations found substantial heterogeneity across studies and identified ceramic fractures and retention loss as the main reasons for failure. It also shows, by the mix of included studies, that occlusal-veneer-specific clinical evidence is still a smaller subset of the broader partial-coverage literature. That is a reasonable inference from the review’s included study pool.
That limitation does not make occlusal veneers a weak option. It simply means clinicians should choose them intentionally, bond them well, and avoid treating them like “mini crowns.” In the wrong case, full crowns still win. In the right case, occlusal veneers win because they are less destructive and still clinically sound.
When full crowns still make more sense
A fair article on occlusal veneers has to say this clearly: full crowns still beat partial coverage in some cases.
Full crowns are usually better when ferrule is non-negotiable
Associated Dental Lab’s crown-lengthening guide says to choose crown lengthening when the intended margin would violate the supracrestal tissue attachment, when isolation is unreliable, or when 1.5 to 2.0 mm of ferrule is required for a full crown on an endodontically treated tooth. If the long-term prognosis depends on circumferential ferrule and axial coverage, a conservative bonded design is no longer the stronger plan.
Full crowns make more sense when the tooth is compromised beyond an occlusal problem
If the tooth is structurally weak apically, mostly buildup, cracked circumferentially, or so subgingival that predictable bonding is unrealistic, a minimal prep posterior restoration may be the wrong answer. ADL’s guidance is explicit here too: if you cannot isolate, do not force a bonded solution. Choose the design that can succeed under the isolation reality you actually have.
Full crowns may also be the better answer when occlusal veneers would overpromise
A 5-year retrospective case series on severe tooth wear found overall adhesive rehabilitation survival of 90.1%, but occlusal veneers specifically had lower estimated survival than facial or palatal veneers, likely because posterior restorations face more fatigue and wear. That does not argue against occlusal veneers. It argues against casual case selection. In some heavy-function cases, full crowns may still be more forgiving if the tooth is already structurally compromised beyond what adhesive posterior restorations can predictably manage.
Material choice for occlusal veneers
Material selection is one of the biggest reasons some occlusal veneers succeed and others disappoint. For most wear cases, the conversation usually comes down to lithium disilicate occlusal veneer versus zirconia occlusal veneer.
Lithium disilicate occlusal veneer
A lithium disilicate occlusal veneer is often the first choice when the case has good adhesive conditions, enough thickness, and a premium esthetic demand. A 2024 study described lithium disilicate occlusal veneers as popular for minimally invasive posterior restoration, which matches how many clinicians use them in practice. Associated Dental Lab’s IPS e.max pages also emphasize shade fidelity, natural translucency, posterior durability, and strong performance, with IPS e.max CAD listed at flexural strength up to 530 MPa.
Lithium disilicate also pairs beautifully with adhesive dentistry. ADL’s bonding guides recommend hydrofluoric acid etching per instructions, followed by silane and adhesive resin cement. That makes a lithium disilicate occlusal veneer especially attractive when the goal is maximum bond reliability on enamel-rich preparations. ADL also notes that IPS e.max is ideal for minimal-prep esthetic work, which supports its role in conservative worn dentition treatment.
Thickness matters, though. In the 2024 fatigue study, 0.8 mm lithium disilicate occlusal veneers outperformed 0.5 mm restorations regardless of whether they were pressed or milled. A separate in vitro study suggested that lithium disilicate occlusal veneers may need more thickness than zirconia to comfortably withstand oral forces. The practical takeaway is not a one-size-fits-all number. It is that lithium disilicate is an excellent choice when the case gives you enough room to respect the material.
Zirconia occlusal veneer
A zirconia occlusal veneer becomes very appealing when the patient has heavy function, reduced restorative space, or a high-stress posterior environment. Associated Dental Lab’s zirconia crown page explicitly positions monolithic zirconia for posterior regions, heavy bite forces, and bruxism because of its fracture resistance and durability. That same high-stress logic carries over naturally to conservative posterior restorations when the design and bonding are handled correctly.
The in vitro data on zirconia occlusal veneers are especially interesting. A 2025 study on ultra-thin translucent zirconia occlusal veneers found promising fracture resistance and favorable wear behavior, with all tested zirconia materials performing well after artificial aging. Another in vitro study found zirconium oxide occlusal veneers to be the most fracture-resistant group tested and suggested that zirconia thickness can sometimes be kept lower than lithium disilicate while still tolerating load.
The tradeoff is bonding strategy. Zirconia is not a glass ceramic. ADL’s guidance is very clear: do not use a silane-only approach. Use air abrasion or sandblasting, MDP chemistry, contamination control, and an adhesive resin pathway when bond strength matters. A zirconia occlusal veneer is often a biomechanically powerful option, but only when the bonding protocol is equally disciplined.
How to choose between lithium disilicate and zirconia
A simple way to think about the choice is this:
- Choose a lithium disilicate occlusal veneer when the case is enamel-rich, esthetics matter, adhesive isolation is excellent, and you have enough thickness for the material.
- Choose a zirconia occlusal veneer when function is heavier, space is tighter, or the posterior load profile pushes you toward a tougher ceramic.
- In either case, let the adhesive strategy drive the workflow from the start rather than treating the intaglio surface as an afterthought.
That framework matches both the material evidence and Associated Dental Lab’s bonding recommendations.
Prep and bonding principles for a minimal prep posterior restoration
Minimal prep does not mean careless prep
A minimal prep posterior restoration is still a restoration with rules. Modern adhesive partial coverage restorations evolved specifically to avoid older retentive features such as isthmuses, proximal boxes, or circumferential shoulders when they are not needed. The idea is to preserve tissue, smooth geometry, and create a preparation that supports adhesive success rather than conventional mechanical retention.
For occlusal veneers, that usually means:
- Preserve as much sound axial structure as possible.
- Round internal angles.
- Reduce only where ceramic thickness, occlusal clearance, or defect removal requires it.
- Keep margins readable and as conservative as the case allows.
- Avoid turning an additive wear case into a crown prep out of habit.
That is the heart of a minimal prep posterior restoration approach.
Immediate dentin sealing may improve bond reliability
Recent laboratory evidence suggests that immediate dentin sealing can improve debonding forces and bond strength in occlusal veneers, even if it does not significantly change fracture resistance. That is useful in worn dentition treatment because many wear cases expose a mixed enamel-dentin substrate. It is not a magic fix, but it reinforces the broader idea that adhesive details matter enormously with occlusal veneers.
Bonding is not optional thinking
Associated Dental Lab’s adhesive playbook is especially valuable here. For zirconia, ADL recommends air abrasion and MDP chemistry. For lithium disilicate, ADL recommends HF etch plus silane plus adhesive resin cement. And ADL explicitly says that partial coverage restorations should be treated as bonding cases. That is exactly how occlusal veneers should be planned from day one.
Workflow: how to make occlusal veneers succeed in real wear cases
Step 1: control the cause before the ceramic
A good tooth wear restoration plan starts before the lab prescription. The systematic review on tooth wear makes this point directly: preventive procedures and measures should be in place before restorative care begins. That means identifying erosion, parafunction, diet, reflux risk, or unstable occlusal habits before definitive restorations go in. Occlusal veneers do not eliminate the cause of wear. They restore the damage.
Step 2: trial the new vertical dimension when needed
In more advanced worn dentition treatment, PMMA prototypes are extremely useful. Associated Dental Lab specifically recommends PMMA for longer wear, vertical dimension trials, and parafunctional patients when adequate thickness and protection are provided. That makes PMMA an excellent bridge between diagnosis and definitive occlusal veneers, especially when the clinician wants to test comfort, phonetics, esthetics, and posterior function before committing to ceramic.
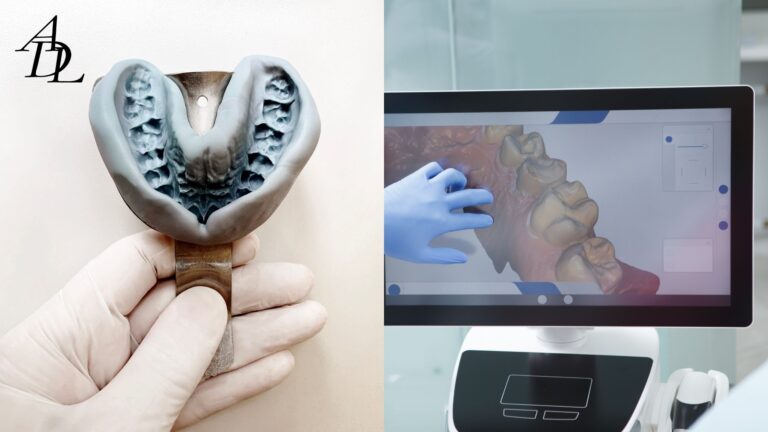
Step 3: choose the right record-capture method
ADL’s scan-versus-PVS guidance is highly relevant to occlusal veneers. Intraoral scanning is ideal for inlays, onlays, and veneers when margins are readable. PVS is favored for subgingival margins, bleeding fields, and soft-tissue-heavy situations. ADL also recommends hybrid workflows when needed, which is a smart point in wear cases because a digital scan may be perfect for most of the case while a conventional backup impression protects the schedule if a margin is questionable.
Step 4: use the lab as part of treatment planning
Associated Dental Lab’s homepage says it plainly: better communication creates better results. ADL emphasizes direct technician communication, digital integration, proven materials, and predictable workflows. In wear cases, that matters because the lab can help evaluate margin readability, occlusal targets, whether a printed verification model is worth using for complex bites, and whether lithium disilicate or zirconia is the safer final choice.
Step 5: seat carefully and protect the result
Occlusal restorations fail faster when seating and protection are rushed. ADL’s occlusion checklist warns that tight interproximal contacts can keep a restoration from fully seating and make occlusion appear falsely high. It also recommends re-checking contacts and occlusion after cementation. After delivery, long-term protection matters too. ADL offers hard, hard/soft, and soft nightguards and specifically frames nightguards as protection for teeth and restorations rather than a cure for bruxism. For many occlusal veneers, especially in parafunctional patients, that protection is part of the restoration plan.
Practical examples: when occlusal veneers beat full crowns
Example 1: generalized posterior erosion with preserved enamel
A patient presents with acid-related cupping and flattened posterior anatomy but relatively intact axial walls and enough enamel for bonding. This is often the classic occlusal veneers case. A full crown would remove healthy circumferential tooth structure mainly to create space that wear has already created. Occlusal veneers beat full crowns here because additive dentistry can rebuild the occlusal table with less sacrifice. A lithium disilicate occlusal veneer may be ideal if esthetics and bonding conditions are strong.
Example 2: full-mouth wear with vertical dimension loss
In a broader worn dentition treatment case, the clinician may need to increase vertical dimension and re-establish posterior support. Here, a staged approach often beats immediate full crowns. PMMA prototypes can be worn for weeks to test adaptation, then definitive occlusal veneers can restore selected posterior teeth once the new scheme feels stable. That kind of stepwise tooth wear restoration is exactly where additive dentistry offers a real advantage over a one-step full-crown reconstruction.
Example 3: heavy-function molar with limited occlusal space
A bruxing patient has a severely worn mandibular molar with minimal restorative thickness available but good overall tooth integrity and manageable margins. In a case like this, a zirconia occlusal veneer may beat a full crown because zirconia tolerates high stress well and may permit a thinner conservative design than lithium disilicate in some setups. The key is that the clinician must use the correct zirconia bonding protocol and deliver a protective guard afterward.
Example 4: deep sulcular box, but no ferrule requirement
A posterior tooth has a deep sulcular margin on one surface but otherwise remains a reasonable adhesive candidate. ADL’s margin guide suggests that if the margin is sulcular, the supracrestal tissue attachment is respected, and rubber dam isolation is achievable, deep margin elevation can be the conservative move. After that, the least invasive adhesive design that meets strength goals should be considered before defaulting to a full crown. In wear-driven cases, that can preserve maximum enamel and keep the restoration in the additive zone.
Example 5: when a full crown clearly wins
An endodontically treated molar has apical structural compromise, unreliable isolation, and needs 1.5 to 2.0 mm of ferrule for predictable long-term service. This is not the case to force into occlusal veneers. ADL’s guidance is explicit that this is where crown lengthening and full coverage may be the safer plan. The conservative option is only better when it is also the durable option.
Common mistakes that make clinicians abandon occlusal veneers too soon
Mistake 1: treating occlusal veneers like tiny crowns
Occlusal veneers are not “short crowns.” They are adhesive partial coverage restorations. When clinicians skip the true bonding workflow, use the wrong intaglio treatment, or rely on cement alone, they turn a bonding case into a compromised retention case. ADL’s cement guide makes this distinction unmistakable.
Mistake 2: choosing a full crown just because the patient is worn
Wear alone is not a reason for circumferential reduction. In fact, the tooth-wear literature points in the opposite direction: worn dentition treatment should be adhesive and additive whenever achievable. If the case still offers enamel, readable margins, and a realistic bonded pathway, jumping straight to full crowns may spend tissue unnecessarily.
Mistake 3: ignoring the limits of the material
A lithium disilicate occlusal veneer and a zirconia occlusal veneer do not behave the same way. Lithium disilicate rewards excellent bonding and adequate thickness. Zirconia rewards high-stress indications and careful MDP-based bonding. Using either material outside its comfort zone is a fast way to blame the concept instead of the case selection.
Mistake 4: scanning a margin the scanner cannot really see
ADL’s digital guidance is very practical here: scanners are excellent for inlays, onlays, and veneers with readable margins, but PVS is favored when margins are subgingival or bleeding persists. Some failures blamed on occlusal veneers are really failures of record capture. Hidden margins do not become clearer because the case is conservative.
Mistake 5: skipping occlusal protection in parafunction
Posterior adhesive restorations in wear cases do better when the load is managed. The severe tooth wear case series showed lower survival for occlusal veneers than for facial or palatal veneers, which makes mechanical protection even more important in heavy-function patients. A professionally designed nightguard is often not an accessory afterthought. It is part of the tooth wear restoration plan.
Conclusion
Occlusal veneers beat full crowns when the case is really a rebuilding problem, not a ferrule problem. They are strongest in worn dentition treatment when enamel remains, margins are manageable, additive dentistry can restore lost anatomy without circumferential destruction, and the clinician is ready to execute a true adhesive protocol. Their biggest advantage is not that they replace every full crown. It is that they let clinicians save more tooth in the cases that do not need full coverage.
They are not a shortcut. They are a disciplined form of tooth wear restoration. Material choice matters. Thickness matters. Occlusion matters. Isolation matters. And case selection matters most of all. When those pieces line up, a minimal prep posterior restoration can outperform a more aggressive plan simply by being kinder to the tooth and still strong enough for the job.
Associated Dental Lab is a dentists’ trusted Full-Service Dental Lab in Los Angeles, crafting smiles since 1962. ADL emphasizes direct technician communication, full CAD/CAM support, proven materials including zirconia and IPS e.max, digital file acceptance for STL, PLY, and OBJ, and practical turnaround windows such as 7 business days for standard crown and bridge, 3 business days for provisional crowns, and 3 to 5 business days for nightguards and retainers. If you want a dentists’ trusted Full-Service Dental Lab to help you plan conservative wear cases, occlusal veneers, partial coverage restorations, and full-mouth workflows, contact us at Associated Dental Lab and let our team help you choose the right restorative path for your next case.
FAQ
Are occlusal veneers better than full crowns for worn dentition treatment?
Occlusal veneers are often better than full crowns for worn dentition treatment when the main problem is lost occlusal anatomy, enough enamel remains for bonding, and the tooth does not require full-crown ferrule. They preserve far more tooth structure, and broader posterior partial-coverage evidence shows short-term performance comparable to full crowns in many cases, though occlusal-veneer-specific evidence remains less mature than crown evidence.
Is a lithium disilicate occlusal veneer strong enough for tooth wear restoration?
A lithium disilicate occlusal veneer can be a very strong tooth wear restoration when thickness and bonding are appropriate. Laboratory evidence shows better fatigue resistance at 0.8 mm than at 0.5 mm in one study, and ADL’s IPS e.max guidance supports lithium disilicate for durable, esthetic posterior use when the adhesive protocol is handled correctly.
When is a zirconia occlusal veneer the better choice?
A zirconia occlusal veneer is often the better choice when restorative space is tight, posterior loads are high, or the patient has heavy bite forces or bruxism. Associated Dental Lab positions zirconia for high-stress posterior cases, and in vitro studies on zirconia occlusal veneers show high fracture resistance and favorable wear behavior. The key is using air abrasion, MDP chemistry, and a proper adhesive workflow.
Why are occlusal veneers considered additive dentistry?
Occlusal veneers are considered additive dentistry because they rebuild worn anatomy with minimal further removal of sound tooth structure. The tooth-wear literature explicitly favors reversible, adhesive, additive approaches whenever achievable, and biologically based management emphasizes preserving the tooth over pursuing aggressive full-coverage reconstruction too early.
Is an occlusal veneer really a minimal prep posterior restoration?
Yes, an occlusal veneer is typically a minimal prep posterior restoration because it uses a non-retentive adhesive design with reduced ceramic thickness rather than a full circumferential crown prep. That does not mean “no rules.” It means the preparation is conservative, material-driven, and designed for bonding rather than traditional mechanical retention.
Do occlusal veneers work for bruxers?
Occlusal veneers can work for bruxers, but the case must be selected carefully. Posterior wear restorations face higher fatigue loads, zirconia may be preferable in some heavy-function situations, and protective nightguard therapy is often part of the long-term plan. ADL offers hard, hard/soft, and soft nightguards specifically to protect teeth and restorations.
When should a full crown still be chosen instead of occlusal veneers?
A full crown should still be chosen instead of occlusal veneers when the tooth needs ferrule, when isolation is unreliable, when the intended margin would violate the supracrestal tissue attachment, or when the tooth is too structurally compromised for a durable bonded solution. In those cases, full coverage is not less conservative in spirit. It is simply more realistic for long-term survival.