In full-arch implant therapy, the step that most reliably prevents costly remakes isn’t fancy ceramics—it’s the rehearsal. A full-arch PMMA provisional (often a milled or printed PMMA provisional) functions as a durable “trial prosthesis implants” stage where you can validate lip support, tooth position, occlusion, VDO verification PMMA, and phonetics try-in dentistry in real life, not just in CAD. Prospective and cohort studies of digitally prefabricated PMMA provisionals for immediate full-arch loading show predictable one-year outcomes, especially when planning and capture are digital from the start. PMC
Why You Should Never Skip a PMMA Try-In
A try-in you can live with—not just look at
- Aesthetics: The PMMA stage verifies midline, smile arc, tooth display at rest/smile, buccal corridor, gingival contours, and “papilla illusions”—with photo and video feedback instead of chairside guesswork. Immediate full-arch protocols that incorporate a prefabricated PMMA show controlled esthetics during healing and functional adaptation.
- Function & occlusion: Chewing, parafunction, and excursions stress-test your scheme before the definitive. Systematic reviews highlight occlusion as a contributor to prosthetic complications in full-arch implant-supported fixed prostheses; controlling it in provisional phases reduces later issues. MDPI
- VDO: Muscles, joints, and speech confirm whether the vertical is truly comfortable. Closest speaking space methods and contemporary VDO reviews remain validated adjuncts to verify vertical dimension. thejpd.org
- Phonetics: Real “F/V” and “S” tests in PMMA expose palatal contour and incisal edge errors that wax often hides; prosthodontic phonetics literature supports using sibilants and labiodental sounds to refine design.
Why PMMA as the material?
Modern PMMA (milled or printed) balances polishability, dimensional stability, and short-term strength. In-vitro and review data show printed PMMA provisional materials can meet or exceed key mechanical benchmarks (flexural strength, hardness, wear) compared with milled PMMA—material- and printer-dependent.
Digital Foundations: Records That Make PMMA Pay Off
Capture implant position with precision
For full-arch accuracy, photogrammetry/stereophotogrammetry consistently demonstrates superior trueness and precision versus conventional intraoral scan stitching across an arch—meeting misfit thresholds for complete-arch prostheses. When available, it simplifies the prefabricated PMMA step and reduces chairside adjustments.
Establish a stable jaw relation and virtual articulation
- Verify CR/MIP with a repeatable record.
- Align with a virtual articulator to set assumptions for guidance and excursions; fine-tune later based on PMMA feedback.
Gather photo and speech baselines
- Frontal/smiling/profile photos under consistent lighting.
- 20–30-second phone video of the patient counting “sixty-seven to seventy-seven,” saying “Mississippi,” and “forty-five/fifty-five.” These phrases give you sibilants and labiodentals for later comparisons.
The Full-Arch Provisional Protocol
Step 1: Pre-planning & Rx clarity
Define esthetic priorities (tooth display, smile arc), functional aim (mutually protected vs controlled group function), and hygiene targets (intaglio contours, cleansability). Include turnaround constraints so the lab can choose printed PMMA provisional for speed or milled PMMA for an extended wear test.
Step 2: CAD design—build what you’ll actually deliver
- Mirror the definitive geometry. Keep wall thickness and access tube positions close to the final so clearances and phonetics in PMMA are honest.
- Document proposed VDO and planned occlusal contacts; tag any areas you expect to adjust so you can confirm them later.
Step 3: Manufacture the PMMA try-in dentures
- Printed for rapid iteration; milled for highest polish/wear if the patient will trial longer. Comparative studies show acceptable marginal fit and occlusal precision from both approaches, with method- and resin-specific differences.
Step 4: The try-in appointment (30–45 minutes)
H3: Esthetic try-in checklist (fast and focused)
- Framing the face:
- Midline with philtrum/facial midline
- Tooth display at rest (≈1–3 mm maxillary) and full smile
- Smile arc parallel to the lower lip
- Buccal corridors present but not dark voids
- Tooth form & proportion:
- Central dominance; progressive embrasures; texture/luster by age/personality
- Gingival/tissue illusions & hygiene:
- Cervical transitions, papilla “shadows,” floss/threader path, water-flosser access
- Documentation:
- Capture the same photo poses and a short speech clip for A/B comparison later
(Emphasizing cleansability in the try-in phase leads to fewer maintenance issues post-delivery.) PubMed
H3: VDO verification PMMA—objective + subjective
- Conversational speech for 2–3 minutes (muscle comfort).
- “Sixty-seven to seventy-seven” (sibilants) to check closest speaking space.
- Gentle chewing simulation to confirm MIP repeatability.
- Quick frontal/profile photos to confirm facial thirds and lower face support.
Classic sources and modern reviews support closest speaking space as a physiologic cross-check for vertical dimension.
H3: Phonetics try-in dentistry—chairside scripts that map to edits
- F/V (labiodental): “forty-five/fifty-five.”
- Dull F/V → lengthen or move maxillary incisors labially to contact the wet-dry line.
- Lip bite/harsh F → shorten or move incisal edges lingually. Wjpmr
- S (sibilant): “sixty-six/seventy-seven/Mississippi.”
- Whistle → reduce the palatal air channel (add palatal bulk behind incisors).
- Lisp → thin palatal contour or shorten incisal edges 0.3–0.5 mm.
Step 5: Short home wear (48–72 hours)
Ask the patient to eat soft foods, speak naturally, and record a 30-second “daily diary” video. Immediate-load PMMA workflows benefit from real-world functional feedback; several cohorts report stable 1-year results when the prefabricated PMMA is used to condition function and esthetics.
Step 6: Capture edits with precision
- Pencil-mark intraorally; photograph; then scan the PMMA try-in dentures with your adjustments.
- Send a concise change list: “Raise #8–9 by 0.5 mm; soften palatal behind 8–10 for S; broaden posterior contacts; shift screw-access 0.5 mm palatal.”
Step 7: Iterate once (sometimes twice) → approve for definitive
Most cases resolve with a single iteration; complex esthetics may need two. In either scenario, you’re locking in esthetics, occlusion, VDO, and phonetics with the PMMA, not gambling on the definitive.
Occlusion, Excursions, and Access Channels in the PMMA Stage
Choose and prove your scheme
For full-arch fixed implant prostheses, a mutually protected scheme—or carefully controlled group function—reduces stress concentrations. Reviews associate occlusal design with prosthetic complications; dialing contacts and guidance in PMMA first reduces ceramic chipping and loosening downstream.
Check screw-access safety and thickness
Use PMMA to confirm your angulation keeps access in low-stress zones (lingual or central fossae) and that there’s adequate bulk around tubes. Chipping at access margins during the trial is a gift—it tells you where to add bulk in the final.
Manage cantilevers
Keep posterior cantilevers conservative and test functionality in PMMA; reinforcement of the final can be planned based on any micro-fractures or wear facets observed during trial.
Printed vs. Milled PMMA: Which to Choose—and When
- Printed PMMA provisional
- Pros: Fastest to fabricate and iterate; validated resins show strong flexural strength and wear in several reviews.
- Use when: You want rapid A/B testing of esthetics/phonetics; short wear periods; early iterations.
- Milled PMMA
- Pros: Dense, highly polishable surface; great for longer provisional phases or “final dress rehearsal.”
- Use when: Patients need several weeks of function or you want the most wear-resistant provisional during conditioning. Comparative data show both methods can achieve acceptable fit and occlusal precision; the choice is case- and lab-specific.
Managing Tissue, Intaglio, and Cleansability
- Verify intaglio relief over multi-unit abutments/bars; avoid impingement and ensure water-flosser/threader access.
- Shape emergence to balance lip support and cleansability; condition tissues during the PMMA phase to inform the final’s contours. Immediate full-arch protocols emphasize hygiene-friendly contours during provisionalization to reduce complications.
Data Capture & Lab Communication That Prevents Remakes
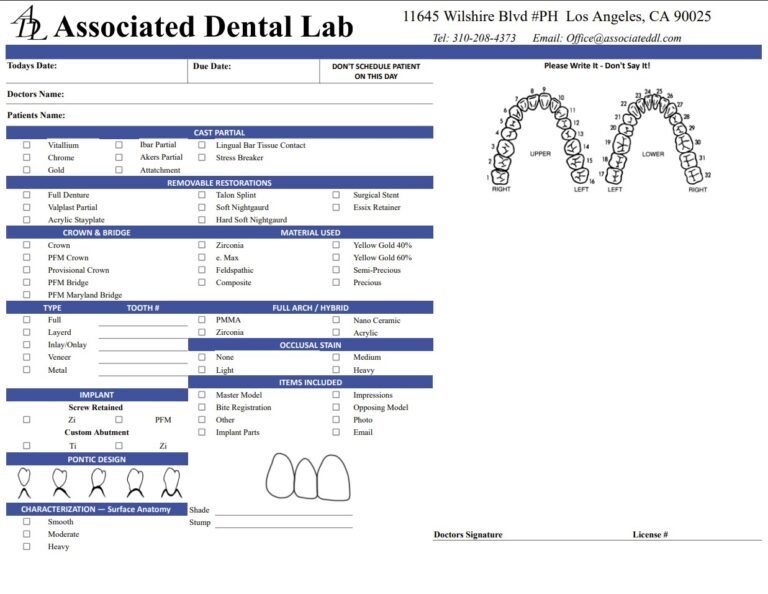
What to send (every time)
- Implant distribution and connection details (and whether photogrammetry was used).
- Proposed VDO and occlusal philosophy.
- Esthetic try-in checklist results (bullet format).
- Phonetic notes tied to specific, measurable adjustments (e.g., “shorten 8–9 by 0.4 mm; thin palatal contour 0.3 mm”).
- Scans of the modified PMMA and synchronized photo set.
What your lab can do to help
A lab that fabricates in-house and supports digital submissions can compress design and remake cycles, particularly when they also offer local pickup/courier and have clear “send a case” instructions. (ADL: local pickup, prepaid shipping, digital scan intake.)
Troubleshooting: Symptom → Likely Cause → Fast Fix
- Lisp on “S” → palatal channel too narrow or edges too close → thin palatal contour or shorten maxillary incisors 0.3–0.5 mm; retest “sixty-seven/seventy-seven.”
- Whistle on “S” → channel too wide → add palatal bulk behind 8–10 to narrow jet; retest.
- Thuddy/unclear F/V → incisal edge not meeting wet-dry line → lengthen/move labially (if dull) or shorten/move lingually (if lip bite).
- “Can’t find my bite” after a few minutes → VDO too high or contacts too point-centric → broaden contacts; confirm MIP after 48-hour wear.
- Access-hole chipping → insufficient bulk or sharp internal angles → thicken around channel; round internal line angles in PMMA before final.
- Posterior soreness/wear facets → occlusal overload or cantilever length → redistribute contacts; shorten cantilever; confirm scheme per the occlusion literature.
Metrics That Matter During the PMMA Phase
- Photo symmetry: midline, cant, smile arc.
- Speech timing: the number of repetitions needed for clear “S” without whistle/lisp.
- Chewing comfort: patient-reported effort and MIP “findability.”
- Hygiene: patient demonstration with threader/water-flosser; plaque disclosure if needed.
- Adjustment count: how many contacts needed change after 48–72 hours (aim to lower this iteration-to-iteration).
Tracking these makes approval for the definitive objective, not just “it looks good.”
Frequently Asked Questions (FAQ)
1) What is a full-arch PMMA provisional, and why not skip it?
It’s a durable prototype that lets you verify esthetics, occlusion, VDO verification PMMA, and phonetics try-in dentistry under real conditions—especially valuable in immediate-load digital workflows, where prefabricated PMMAs have shown stable 1-year clinical outcomes.
2) Are PMMA try-in dentures strong enough for short-term function?
Yes. Multiple reviews and studies report clinically acceptable flexural strength and wear resistance for both printed and milled PMMA provisional materials; selection is resin/printer dependent.
3) Should I choose printed PMMA provisional or milled for my first try-in?
Print for speed and iteration; mill for extended provisional phases or when you want the most polish/wear resistance. Both can achieve acceptable fit and occlusal precision with validated workflows.
4) How do I confirm VDO in the PMMA?
Use a multi-factor method: sibilant “S” closest speaking space, conversational comfort, and repeatable MIP—classic methods validated in the literature and reinforced by modern reviews.
5) Which occlusal scheme is best for full-arch fixed prostheses?
Most clinicians aim for mutually protected occlusion (or carefully controlled group function); reviews link poor occlusal design with higher prosthetic complication rates. Validate your scheme in PMMA first.
6) Does photogrammetry really help here?
Yes. Studies show stereophotogrammetry/photogrammetry improves full-arch implant impression precision versus cross-arch IOS stitching, helping prefabricated PMMAs seat accurately with fewer adjustments.
7) How does the lab keep my full-arch provisional protocol on schedule?
By fabricating in-house, accepting digital submissions, and offering local pickup/courier options. Associated Dental Lab provides these logistics so you can iterate quickly without losing calendar time.
Conclusion
Treat the full-arch PMMA provisional as a clinical instrument, not a formality. Use it to prove esthetics (with an esthetic try-in checklist), to confirm functional comfort and closest speaking space for VDO verification PMMA, to tune phonetics with targeted palatal and incisal adjustments, and to finalize occlusion before committing to the definitive. The evidence base behind prefabricated PMMA in immediate full-arch workflows, the precision advantage of photogrammetry for cross-arch capture, and modern provisional material science all point the same way: a structured PMMA phase is the safest path to high-confidence finals with minimal chairside drama.
About Associated Dental Lab
Associated Dental Lab is a dentists’ trusted Full-Service Dental Lab in Los Angeles. They accept digital files from major IOS platforms, streamline “Send a Case,” offer local pickup and prepaid shipping, and fabricate in-house for reliable turnarounds—ideal when you’re iterating full-arch cases from PMMA through to definitive. Contact them to coordinate your next case.