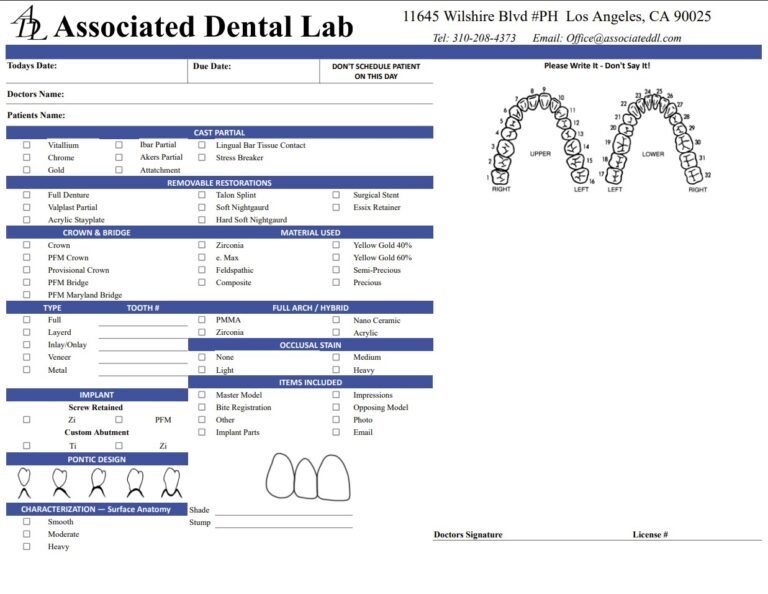
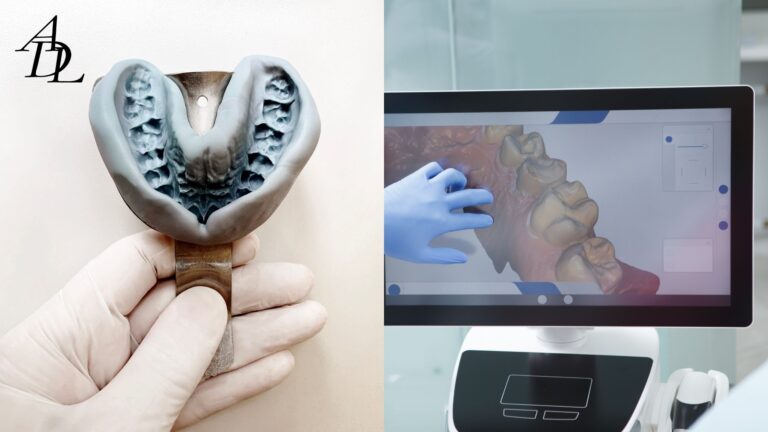
The rise of dental photogrammetry and intraoral scanning has transformed how clinicians capture implant positions—especially in full-arch cases where microns matter. Photogrammetry specialized systems triangulate the 3D coordinates of implant heads with arrays of calibrated photos, while intraoral scanners (IOS) create high-resolution meshes of soft tissue, teeth, and prosthetic contours. Used alone, each modality has strengths and limits. Used together as a hybrid workflow, they can reduce chair time, increase full-arch scan accuracy, and speed the path to a passive prototype or definitive restoration.
In the last few years, multiple systematic reviews and in-vitro/in-vivo studies have compared photogrammetry vs IOS for complete-arch implants. The consensus trend is clear: stereophotogrammetry (SPG) often shows higher trueness and precision for the 3D position of implants across a full arch, while IOS excels at capturing soft-tissue architecture, occlusal detail, and tooth morphology—both of which are essential for esthetics and functional prosthesis design. PMC
Core Concepts: What Each Modality Does Best
Dental photogrammetry (SPG)
- Captures the 3D position and angulation of multiple implants across a full arch with sub-millimetric precision.
- Less sensitive to edentulous scan stitching and field length than IOS when the goal is accurate implant coordinates for passivity.
- Recent reviews and meta-analyses report SPG trueness/precision advantages over IOS for complete-arch implants, though high-quality clinical trials are still accumulating.
Intraoral scanning (IOS)
- Captures soft tissue, bite, tooth surfaces, and prosthetic contours efficiently.
- In many situations—including single units and short spans—IOS matches or exceeds conventional impressions; for full arches, results depend on scan strategy, scanner, and geometry. PubMed
Why a hybrid?
- SPG locks in implant coordinates.
- IOS supplies the peri-implant and occlusal context, smile line, and emergence contours.
- Together, the datasets reduce the uncertainty that appears when you stretch any one technique beyond its sweet spot. Systematic reviews favor this division of labor for photogrammetry dental implants steps in complete-arch workflows.
Evidence Snapshot: Photogrammetry vs IOS
- A 2025 systematic review/meta-analysis found SPG showed higher accuracy than IOS for complete-arch implant impressions in most included studies.
- Additional reviews echo higher trueness/precision for stereophotogrammetry in complete-arch scenarios, while calling for more homogeneous clinical trials. Wiley Online Library
- Studies continue to probe implant scan bodies—their geometry, length, and orientation can materially affect IOS accuracy in full-arch scans. Shorter or simplified designs and optimized geometries have demonstrated better alignment precision in certain conditions. MDPI
- Not all research agrees; some in-vitro or clinical reports show IOS or conventional methods performing well under controlled protocols. The practical takeaway: match the capture method to the span, number of implants, tissue conditions, and restoration stage.
A Decision Tree for Hybrid Workflow Implants
Start Here—Patient and Case Context
Ask these questions before you choose the pathway:
- How many implants and what span?
- 1–2 implants, short span with adjacent teeth → IOS-first path is typically adequate.
- 3–6 implants full arch (All-on-X) → favor photogrammetry for coordinates plus IOS for soft tissue.
- What is the edentulous extent?
- Fully edentulous arches amplify IOS stitching error risk over long spans; SPG reduces that risk.
- Is the case at prototype/verification or at final?
- Early prototype stages benefit the most from precise coordinates to reduce adjustments later.
- Are there access/angulation challenges?
- Divergent implants or limited vertical space may benefit from SPG’s coordinate capture, then IOS for emergence/gingival detail.
Branch A — Single-Unit and Short-Span
If: 1–2 implants, stable soft tissue, clear opposing dentition
Then:
- Capture with IOS using validated implant scan bodies; follow the scanner’s full-arch vs quadrant recommendations.
- Use manufacturer-matched scan bodies or verified cross-platform libraries; improper library/brand mixing can introduce alignment error.
- Verify with a printed model or try-in as needed.
Why: For short spans, clinical studies and reviews show IOS performs predictably with the right scan bodies and scan path.
Branch B — Full-Arch, 4–6 Implants (All-on-X)
If: complete-arch rehabilitation or long spans
Then:
- Use dental photogrammetry to acquire implant positions (coordinates/angulations).
- Immediately follow with an IOS of soft tissue, palate/vestibule, opposing arch, and bite.
- Fuse the datasets in CAD (SPG coordinate file + IOS mesh).
- Optional: add a rigid printed prototype or verification device if the literature threshold (e.g., angular deviation ≤1° for passive fit) is mission-critical in your case.
Why: Meta-analytic data favor SPG for full-arch scan accuracy of implant positions; IOS supplies the tissue and occlusal information needed for esthetics and phonetics.
Branch C — Hybrid Under Time Pressure
If: minimal chair time is available or patient tolerance is limited
Then:
- SPG first (fast coordinate capture), then a streamlined IOS (tissue and bite).
- If IOS quality is compromised, consider a quick desktop scan of a prototype with pick-up cylinders as a safety net.
Why: SPG systems can capture coordinates rapidly, and modern IOS devices can complete context scans efficiently; together they minimize resets.
Step-By-Step Hybrid Workflow (Chairside + Lab)
1) Pre-op planning
- Confirm implant platforms and brands; ensure compatible implant scan bodies and photogrammetry targets are available.
- Standardize photo protocol (retracted, frontal, lateral, shade tab).
- Schedule enough time for SPG + IOS in one visit to avoid tissue changes between captures.
2) Photogrammetry capture (implants only)
- Place the photogrammetry targets per system IFU; capture sequences until software reports stability.
- Export the coordinate dataset (usually CSV/JSON + STL reference).
- Advantages demonstrated in recent reviews/studies: reduced angular/linear error across the arch compared to IOS alone for implants.
3) Intraoral scan (tissue/occlusion context)
- Scan soft tissue, emergence profiles, opposing arch, and bite.
- Choose scan bodies with geometries validated for your scanner (length, dome/flat features, anti-rotation). Evidence shows geometry and even length can influence implant alignment accuracy.
- Use a full-arch strategy that minimizes stitching breaks in edentulous spans.
4) Data fusion at the lab
- Your lab merges SPG coordinates with the IOS mesh in CAD.
- The result is a master reference for digital workflow dentistry: accurate implant positions + detailed soft tissue and occlusion.
- Associated Dental Lab accepts direct digital submissions (DS Core, DEXIS, iTero, Medit, TRIOS) and coordinates hybrid cases daily, which simplifies this step.
5) Printed prototype / verification (strongly recommended in early cases)
- Print a rigid prototype with multi-unit abutments or verification cylinders; assess passivity (Sheffield test) and make phonetic/esthetic notes.
- Several studies recommend a rigid try-in as a practical safeguard while the evidence base continues to mature. ResearchGate
6) Final design & delivery
- Proceed to milled/printed frameworks (e.g., Ti-bar with wrap, monolithic zirconia) after prototype sign-off.
- Maintain a digital archive to enable fast remakes.
Practical Tips That Improve Accuracy (Regardless of Path)
Optimize scan-body selection and libraries
- Use brand-matched scan bodies and current library versions. Research shows geometry and length materially affect precision; short or simplified geometries may reduce error in specific scanners.
Control the scan path
- For IOS full arches, choose a path that avoids long return jumps and includes stable features (palate/crest). Small technique choices compound over spans (recent work continues to analyze scan pattern effects).
Watch your “hand-offs”
- Fusion errors often come from mismatched or outdated libraries. Lock your clinic + lab on the same target, body, and library versions for the entire case.
Build in a verification step
- A one-appointment rigid prototype try-in reduces downstream framework adjustments and helps meet the “passive fit” expectation highlighted in reviews.
Common Hybrid Patterns (With Examples)
Pattern 1 — Edentulous Maxillary All-on-X
- Capture: SPG (implant coordinates), then IOS for tissue and bite.
- Prototype: rigid printed multi-unit try-in; refine vertical, smile arc, and phonetics.
- Why: Maximizes coordinate accuracy and esthetic tunability. Meta-analysis favors SPG for the coordinate job.
Pattern 2 — Mandibular Full-Arch with Limited Time
- Capture: SPG first (fast), then focused IOS (lingual flange and occlusion).
- Prototype: printed long-term PMMA with titanium base interfaces.
- Why: Minimizes intraoral time where saliva and tongue mobility can degrade long IOS sequences.
Pattern 3 — Short-Span with Adjacent Teeth
- Capture: IOS only using validated scan bodies and libraries.
- Prototype: optional; printed model check if contacts or emergence are uncertain.
- Why: Literature supports IOS for short spans; photogrammetry not necessary.
Speed vs Accuracy: What the Studies Suggest
- Accuracy: Strong trend toward better implant coordinate trueness/precision with SPG for complete arches, while IOS can perform well in specific protocols and is excellent for context data.
- Speed and tolerance: SPG sequences are typically quick; IOS time varies with arch length and operator technique.
- Emerging tech: Novel scan body concepts (reverse scan bodies; modified geometries) and even smartphone-based photogrammetry proofs of concept are being studied; results are promising but should be adopted with caution until broadly validated.
Cost, Equipment, and Team Training
Equipment considerations
- Dedicated photogrammetry systems represent an investment; evaluate case volume and whether your lab can provide chairside assistance or rental models for ramp-up.
- Ensure your IOS is updated and that your team follows the manufacturer’s long-span scan path guidance.
Training plan (four weeks)
- Week 1: Team in-service on scan body placement, library matching, and SPG capture steps.
- Week 2: First two hybrid cases with lab on standby via video chat.
- Week 3: Add rigid prototype try-in to your default protocol.
- Week 4: Review outcomes (seat time, adjustments, remake rate) with your lab; refine.
Quality Assurance: Metrics to Track with Your Lab
- Coordinate deviation at verification (framework passivity notes).
- Remake and redo rate for full-arch implants by capture method.
- On-time rate and number of clarification emails (communication efficiency).
- Seat-visit duration and number of post-delivery adjustments.
A KPI-driven lab partner will share weekly snapshots and help you segment hybrid vs non-hybrid outcomes. Associated Dental Lab emphasizes on-time delivery, technician communication, and digital intake—useful if you want a partner already configured for these checkpoints.
Frequently Asked Questions (FAQ)
1) When is dental photogrammetry clearly better than intraoral scanning?
In complete-arch implant cases where sub-millimetric coordinate accuracy drives passivity. Multiple reviews show stereophotogrammetry yielding higher trueness/precision than IOS for full arches. Use IOS for soft tissue, occlusion, and esthetics.
2) Can IOS alone work for full arches?
Sometimes—protocols, scan paths, and scan bodies matter. Some clinical studies show excellent results with IOS, while others highlight accuracy limits over long spans. A rigid verification try-in is a prudent safeguard.
3) What about implant scan bodies—do they really change accuracy?
Yes. Geometry, height, and library fidelity influence trueness/precision in complete-arch IOS. Shorter or simplified geometries have shown advantages in some studies; always match libraries and versions with your lab.
4) How do I fuse photogrammetry and IOS files?
Your lab merges SPG coordinates with the IOS mesh in CAD. Send both datasets in the same case with clear notes on abutment types and occlusal records. ADL accepts direct digital submissions from major IOS platforms.
5) Does photogrammetry add chair time?
Capture is typically quick; the total appointment is often shorter than long IOS attempts on edentulous arches. You’ll usually save time at verification and delivery by reducing adjustments. (Your mileage depends on team familiarity.)
6) Are smartphone photogrammetry solutions ready?
Early in-vitro/in-vivo data are emerging; some reports suggest clinically acceptable accuracy for complete-arch implant capture in controlled workflows, but widespread validation is ongoing. Proceed thoughtfully.
7) What’s the safest way to start with hybrid workflow implants?
Begin with SPG + IOS on your next All-on-X case, insist on a rigid prototype try-in, and perform a structured debrief with your lab after delivery to lock in lessons learned.
Conclusion
Choosing between dental photogrammetry and intraoral scanning is not either-or. For complete-arch implant rehabilitation, SPG anchors the coordinate truth while IOS delivers the tissue and occlusal reality. This hybrid approach—supported by current evidence—reduces risk, improves full-arch scan accuracy, and shortens the path to passive frameworks and beautiful finals. Build your decision tree around span length, edentulism, angulation, and stage of treatment, and you’ll know when to deploy SPG, when IOS is enough, and when to fuse both for the win.
About Associated Dental Lab
Associated Dental Lab is a dentists’ trusted Full-Service Dental Lab in Los Angeles (since 1962), supporting digital workflow dentistry for implants, crowns & bridges, removables, and guards. ADL accepts digital scans from DS Core, DEXIS, iTero, Medit, and TRIOS; offers local pickup and prepaid shipping; and provides technician-to-doctor communication to streamline hybrid workflow implants from planning through delivery. If you’re ready to standardize a photogrammetry + IOS protocol with an experienced partner, contact Associated Dental Lab and send a case today.