If you don’t measure it every week, you can’t manage it next week. High-performing practices use a simple, shared dashboard with their lab to track dental lab KPIs—not once a quarter, but weekly—so they can catch small problems (tight contacts, late deliveries, inconsistent shades) before they become big ones. The same mindset applies to dental practice KPIs on the clinic side: case acceptance, schedule utilization, and reappointment rates. When the lab and clinic look at one scoreboard, chair time shrinks, remakes drop, and patients notice smoother visits. Leading practice-management bodies frame KPIs as the measurable values that help owners assess growth, profitability, and operational health; in dentistry, translating those KPIs into lab-clinic workflows is where the real leverage lives. ADA
This guide gives you a complete weekly KPI framework focused on three outcomes that move the needle: remake rate dentistry, on-time case delivery, and redo rate dental lab, with supporting metrics like lab turnaround time, case acceptance rate, and lab communication metrics. You’ll get field-tested definitions, formulas, targets, examples, and a ready-to-use dashboard template—plus how to stand it up with your current lab (or with Associated Dental Lab if you want a partner already set up for digital intake, local pickup, and prepaid shipping).
Why Weekly? The Compounding Effect of Small Wins
- Faster feedback: A weekly cadence identifies trends after 10–30 cases, not 10–12 weeks.
- Operator coaching: You can connect adjustments (e.g., better photos, revised Rx instructions) to next week’s outcomes.
- Patient experience: Consistent on-time delivery reduces reschedules and interruptions, improving acceptance and reviews.
The practice literature stresses that KPIs are only useful when they drive decisions—week by week—rather than annual retrospectives that arrive too late to help. Dental Economics
The Six KPIs That Belong on Every Weekly Dashboard
1) Remake Rate (Dentistry + Lab)
Definition: % of cases requiring a remake before permanent delivery (exclude patient-initiated esthetic change requests where clinical quality met the Rx).
Formula: Remakes ÷ Total cases delivered (week) × 100.
Targets & context: Reports and surveys suggest many dentists self-report <2% remake rate, yet a notable minority report ≥4%; lab posts cite ~4% for traditional workflows with lower rates in digital. Benchmarks vary by case mix and digital adoption. PMC
How to use it:
- If rate rises, drill into cause codes (impression/scan error, margin readability, contact/occlusion, shade communication).
- Pair with “First-Pass Fit %” (see below) and “Contact/Occ Recall Tags” for precise coaching.
2) Redo Rate (Post-Delivery Corrections)
Definition: % of delivered cases needing post-seat correction or remake within 90 days for clinical reasons (exclude trauma or new caries).
Why it matters: Redos consume chair time, disrupt the schedule, and erode patient trust. Track them separately from pre-delivery remakes so root causes are clear.
3) On-Time Case Delivery %
Definition: % of cases arriving on or before the promised date.
Formula: On-time cases ÷ Total shipped cases × 100.
Why it matters: Late arrivals cascade into broken appointments and rebookings. Many labs publish standard lab turnaround time expectations by product (e.g., 5–7 business days for common fixed cases; faster for digital), but your KPI should reflect your actual promise dates, not generic averages. Pro Craft Dental Lab Blog
4) Lab Turnaround Time (Calendar Days)
Definition: Days from scan/impression receipt to lab ship or in-hand date.
Break out by: product category (single-unit crown, bridge, removable, implant), and by submission type (digital vs conventional), as digital often ships faster.
5) First-Pass Fit %
Definition: % of cases that seat with no adjustments beyond normal finishing (i.e., margins verified, contacts “snap,” occlusion within two minor marks).
Why it matters: It’s the single best “experience” metric, correlating with fewer remakes, shorter seat visits, and better reviews.
6) Case Acceptance Rate (for lab-dependent treatment)
Definition: % of proposed lab-related treatment ($ or cases) that patients accept.
Formula: Accepted ÷ Proposed × 100.
Why it matters: Acceptance connects your clinical communication and lab esthetics/consistency to revenue. Practice sources commonly highlight acceptance as a pivotal KPI to track habitually. Madras Accountancy
Support Metrics That Explain the Big Six
Lab Communication Metrics
- Complete Rx %: Cases with fully completed lab prescriptions, attachments, and shade/pose photos on first submission.
- Clarification Ping Rate: % of cases where the lab must contact the office to clarify Rx.
- Photo Sufficiency Rate: % of esthetic cases with lab-approved photos (frontal, lateral, retracted, shade tabs).
Communication quality is one of the cleanest leading indicators of remakes and late deliveries. Operational articles for labs explicitly point to KPIs such as remake rate as the technician-level metric that ties daily work quality to outcomes. info.whipmix.com
Clinical Quality Flags
- Margin Readability Score (internal audit)
- Scan Quality Score (digital noise, stitching errors)
- Shade Agreement at Try-In
Pattern recognition here reduces redo friction next week.
Patient Impact
- Seat Visit Duration (avg minutes)
- Unplanned Seat Re-appointments
- Satisfaction notes (from follow-up calls/texts)
Building the Weekly KPI Dashboard (Structure + Formulas)
H2: Data Sources
- Practice management/EHR: production, scheduling, chair time, acceptance.
- Lab portal/CSV: ship dates, remake tags, delivery status.
- Manual entries: try-in outcomes, photo sufficiency, “first-pass fit” tallies.
ADA and Dental Economics pieces emphasize the management value of consistent, business-grade KPI tracking for practices; the trick is mapping those KPIs to lab events every week. ADA
H3: A Simple Weekly Layout (example)
Top row (scorecards):
- Remake Rate %, Redo Rate %, On-Time %, First-Pass Fit %, Avg Turnaround (days), Case Acceptance %.
Trend row (sparklines): 8-week trend for each.
Drill-downs: - By product (PFZ, monolithic zirconia, e.max, full denture, partial, implant crown/bridge).
- By source (Doctor A, Doctor B, hygienist-driven whitening, etc.).
- By submission (digital vs conventional).
Root causes: - Contact tight/loose, occlusion heavy, margin open, shade mismatch, impression/scan issue, Rx incomplete.
H3: Formulas that hold up
- On-time %:
COUNTIF(shipped_on_or_before_due, TRUE) / COUNT(all_shipped) - Avg TAT (days):
AVERAGE(ship_date – received_date) - First-Pass Fit %:
COUNT(first_pass_flag=TRUE) / COUNT(seated_cases) - Case Acceptance % ($):
SUM(accepted $)/SUM(proposed $)
Targets and Benchmarks (Use as Starting Points, Not Absolutes)
- Remake rate dentistry: Aim for ≤2–3% overall; investigate ≥4% sustained for two weeks. Peer-reviewed practice data and lab posts cite values in this range, with better performance common in dialed-in digital workflows.
- Redo rate dental lab: ≤1–2% within 90 days (case-mix dependent).
- On-time case delivery: ≥95% is a practical target; many labs publish turnaround standards—set promise dates you can consistently meet.
- Lab turnaround time: segment by product; digital should outperform conventional.
- First-Pass Fit %: ≥80% (single-unit fixed) and ≥70% (multi-unit) are achievable with strong Rx discipline and photo packs.
- Case acceptance rate: 70–85% for everyday dentistry is frequently cited in practice sources; calibrate by case type.
Using the Dashboard to Cut Remakes and Redos
Focus Area 1: Rx and Photo Discipline
Action: Implement a “complete Rx” gate: the case doesn’t leave the op until the checklist is green (tooth numbers, material, shade, stump shade, reduction photos, bite, opposing, prep photos with retraction, smile poses). Labs and practice literature agree: complete, high-quality inputs correlate with fewer remakes and faster lab turnaround time.
Focus Area 2: Impression/Scan Quality
Action: Track scan rescans, stitching artifacts, and impression retakes; tie to remake/redo root causes. Flag any doctor whose scan defect rate is >1 SD from the mean; coach on retraction, scan path, or material selection. (Technique variation is a known factor in remake variability.)
Focus Area 3: Shade & Esthetics
Action: Require a standardized shade protocol with neutral-light photos and incisal edge tabs; note “shade clarification” pings as a communication KPI. Every additional email adds days and invites late deliveries.
Focus Area 4: Promise Dates You Can Keep
Action: Set promise dates with explicit buffer based on product and historical performance. Monitor on-time case delivery weekly; if <95% for two weeks, renegotiate buffers or modify submission cut-offs (e.g., noon for same-day receipt).
Closing the Loop with Your Lab (Cadence & Playbooks)
Weekly 15-Minute Huddle (Clinic + Lab)
Agenda:
- Review the Big Six KPIs.
- Highlight three cases (one win, two misses).
- Confirm one process tweak for next week (e.g., new photo card, trimming Rx choices, earlier shade confirmations).
Lab-facing articles stress using operational KPIs (not just finance) so technicians can see how their daily work affects outcomes—remake rate is perfect for this.
Monthly Deep-Dive
- Compare digital vs conventional performance.
- Review product-level trends (e.g., implants vs single-unit ceramics).
- Align on staffing or scheduling changes during peak seasons.
Practical Examples (From Dashboard to Action)
Example 1: Remake Spike in Posterior Zirconia
KPI change: Remake rate up to 4.5% over two weeks; cause code = “tight contact/rocking.”
Investigation: Trend is concentrated in cases with dual-arch trays. Literature notes technique can influence remake variability in crowns; switch to full-arch or improved bite records for flagged indications. Result: Remake rate falls to 2.1% in three weeks.
Example 2: On-Time % Slips to 90%
KPI change: Late by 1–2 days on multi-unit bridges.
Fix: Lab surfaces a porcelain-oven bottleneck on Thursdays; practice moves scan submissions for bridges to Monday–Tuesday and adds explicit due-date buffers. Result: On-time back to 96% for the month.
Example 3: Case Acceptance Stagnates at 62%
Signal: Many esthetic cases lack smile-pose photos and a calibrated shade plan.
Change: Add a two-minute “photo starter pack” to treatment-plan consults and include mock-up renders from recent lab cases. Result: Acceptance climbs to 74% in five weeks, consistent with practice KPI literature highlighting acceptance as a priority metric.
Implementation Guide (Step-by-Step)
Week 0 — Prep
- Pick your KPIs (the Big Six).
- Map data sources and owners (who updates which numbers every Friday by noon).
- Define cause codes for remakes/redos (≤8 codes to keep entry fast).
Week 1 — Launch
- Build a one-page dashboard (Google Sheets or BI tool).
- Establish your weekly huddle with your lab.
- Start with current promise dates; don’t change SLAs yet.
Weeks 2–4 — Stabilize
- Audit 10 random cases each week for Rx completeness and photo sufficiency.
- Adjust buffers where <95% on-time persists.
- Begin coaching on outlier scan/impression quality.
Weeks 5–8 — Optimize
- Add First-Pass Fit %.
- Pilot a “no-clarification” goal: aim to cut lab communication metrics pings by 25% through better Rx defaults.
- Revisit cement/provisional protocols if redo causes point there.
Technology Tips: Make the Dashboard Automatic(ish)
- Practice software export: Most systems export schedules, production, and acceptance; automate with a saved report.
- Lab portal CSV: Ask your lab for a weekly CSV (received date, promised date, ship date, cause codes); many labs will generate it on request.
- Templates & defaults: Pre-fill Rx forms with your standard materials and shades to reduce clarification pings.
- Digital submissions: Digital intake commonly improves lab turnaround time; segment your analytics by digital vs conventional to quantify the lift.
What “Good” Feels Like After 90 Days
- Remake rate dentistry: ≤2–3% across case types, with stable cause-code distribution.
- On-time case delivery: ≥95% for three straight months.
- Redo rate dental lab: trending down and isolated to specific, addressable causes.
- Lab turnaround time: predictable by product; digital consistently faster.
- Case acceptance rate: climbing toward your target range (e.g., 70–85% depending on case mix).
- Lab communication metrics: clarification pings cut by ~25–40% from baseline.
Frequently Asked Questions (FAQ)
1) Which dental lab KPIs matter most each week?
Track remake rate dentistry, redo rate dental lab, on-time case delivery, lab turnaround time, first-pass fit %, and case acceptance rate. These KPIs directly affect chair time, patient satisfaction, and profitability.
2) How do we define a remake vs a redo?
A remake happens before definitive delivery; a redo happens after delivery within a set window (e.g., 90 days) for clinical reasons. Separating them clarifies where the process broke and who owns the fix. Lee Ann Brady, DMD’s Dental Blog –
3) What is a reasonable benchmark for remake rate?
Aim for ≤2–3% overall; investigate sustained rates ≥4%. Peer-reviewed and industry sources report ranges from <2% to >4%, influenced by technique and digital adoption.
4) How do we improve on-time case delivery?
Lock in complete Rx packets, use digital submissions when possible, and set promise dates with buffers based on product and your lab’s documented lab turnaround time. Review misses weekly with your lab.
5) Which dental practice KPIs connect to lab performance?
Case acceptance, seat-visit duration, unplanned reappointments, and satisfaction notes. Practice sources emphasize tracking acceptance and operational KPIs to drive timely course-corrections. Dental Economics
6) Should we track communication as a KPI?
Yes. Monitor lab communication metrics like “clarification ping rate” and “complete Rx %.” Reducing back-and-forth shortens cycle times and cuts remakes. Lab-operations content explicitly highlights operational KPIs such as remake rate to connect daily work to outcomes.
7) How often should we review the dashboard?
Weekly for the main scorecard; monthly for deeper product and provider trends. Weekly reviews are frequent enough to drive actionable changes without analysis paralysis.
Conclusion
A weekly, shared dashboard aligns your team and your lab around the outcomes patients feel: on-time delivery, smooth seats, and fewer reappointments. Start with the Big Six—dental lab KPIs tied to remakes, redos, on-time %, turnaround, first-pass fit, and dental practice KPIs like case acceptance—and insist on root-cause clarity. When you pair disciplined inputs (complete Rx, better photos, clear promise dates) with weekly accountability, you de-risk your schedule and create a quieter, more predictable restorative lane.
About Associated Dental Lab
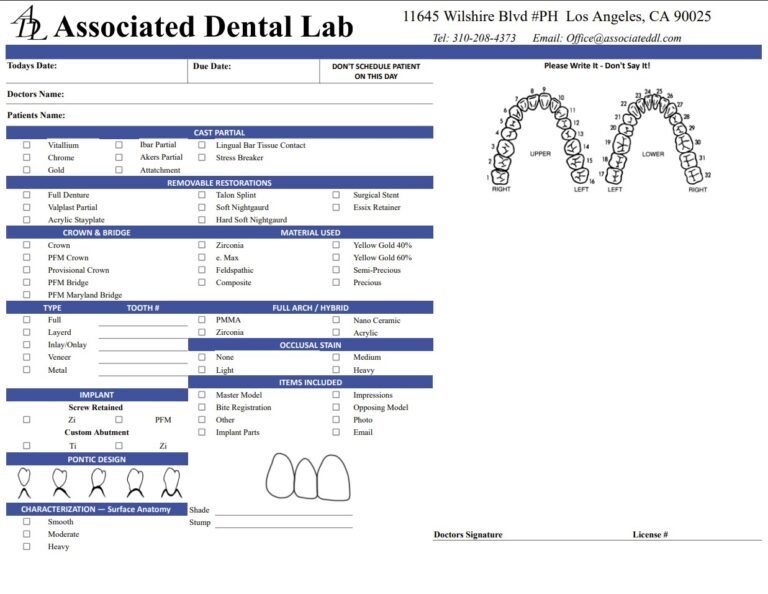
Associated Dental Lab is a dentists’ trusted Full-Service Dental Lab in Los Angeles. They accept digital and traditional cases, provide downloadable Rx slips, local pickup, and prepaid shipping, and fabricate restorations under rigorous in-house QC—making it easier to track on-time delivery and reduce remakes with clean handoffs. If you want a lab partner that supports KPI-driven workflows and weekly reviews, contact Associated Dental Lab and send your next case with confidence.